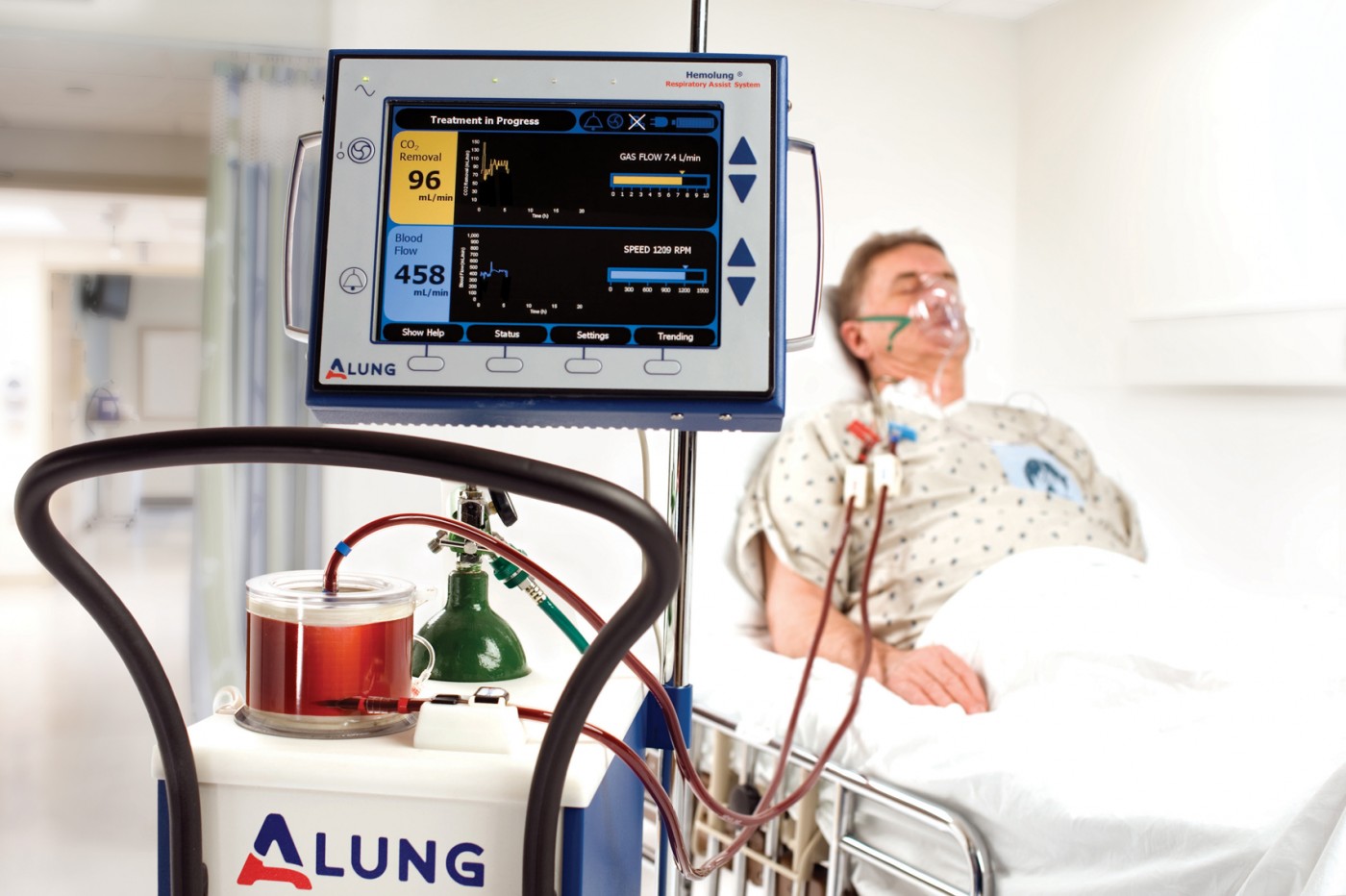
 When Jon Sacker, a 33-year-old cystic fibrosis patient from Moore, Oklahoma, was too sick for a lifesaving double lung transplant, clinicians at University of Pittsburgh Medical Center decided he was going to be the first person in the United States to be connected to the Hemolung Respiratory Assist System. “Jon was in very critical condition when he came to Pittsburgh, and the Hemolung was a lifesaver for him while waiting for his second lung transplant,” said Mario Crespo, MD, who was Mr. Sacker’s pulmonologist, in a news release from UPMC.
When Jon Sacker, a 33-year-old cystic fibrosis patient from Moore, Oklahoma, was too sick for a lifesaving double lung transplant, clinicians at University of Pittsburgh Medical Center decided he was going to be the first person in the United States to be connected to the Hemolung Respiratory Assist System. “Jon was in very critical condition when he came to Pittsburgh, and the Hemolung was a lifesaver for him while waiting for his second lung transplant,” said Mario Crespo, MD, who was Mr. Sacker’s pulmonologist, in a news release from UPMC.
Just two years earlier, Mr. Sacker received a set of lungs, but his body rejected the transplant. While he was waiting for a second transplant, his carbon dioxide levels spiked, making it too risky for another lung transplant. “I though I had brought my husband here to die,” said Sallie Sacker.
Clinicians at UPMC were not going to give up the fight to keep Mr. Sacker alive. “Jon had previously been very active and fit, and we knew we had to do whatever it took to help him,” said Christian Bermudez, MD, chief of UPMC’s Division of Cardiothoracic Transplantation. In February he was connected to the Hemolung, and in March he underwent his transplant surgery.
The Hemolung filters carbon dioxide from the blood and provides oxygen, alleviating the lungs of the burden and allowing them to rest and heal. Typically during a transplant operation, this gas exchange is accomplished through extracorporeal membrane oxygenation, but Mr. Sacker was too sick for the mechanical device. “We had seen the Hemolung Respiratory Assist System used in other countries and wanted to do whatever we could to help this patient,” said Peter DeComo, chairman and chief executive of ALung Technologies, who produces Hemolung.
Hemolung is not currently approved for use in the United States, but Drs. Bermudez and Crespo worked with Diana Zaldonis, MPH, BSN, to notify the Food and Drug Administration of their intent and to receive emergency approval from local hospital officials. Mr. DeComo drove to Toronto in the middle of the night to pick up the closest Hemolung available. “The entire series of events that led to this transplant and Jon’s recovery have been amazing,” said Dr. Bermudez.
All is well for Mr. Sacker, who will remain in Pittsburgh while he recovers. He looks forward to returning to everyday activities, such as running and public speaking. He is also penning the book Imperfect Perfection and will continue to spread the word about organ donation. “Out of all the transplant centers we could have come to, we came here to Pittsburgh,” said Mr. Sacker. “It’s a miracle that’s just not explainable. You just have to thank God.”
For the team who treated Mr. Sacker, it’s all in a day’s work. “Jon’s story is a tremendous example of the depth of the work we do here every day. Most hospitals across the country couldn’t handle a situation as complex as Jon’s, but we can because of our collective experience and an extensive team that includes transplant surgeons, pulmonologists, nurses, and so many more,” said James Luketich, MD, chairman of the Department of Cardiothoracic Surgery.
ALung Technologies, which was founded by William Federspiel, PhD, director of the Medical Devices Laboratory at the McGowan Institute for Regenerative Medicine and Brack G. Hattler, MD, former chief of lung transplant at UPMC, commercialized the Hemolung after it was developed by Dr. Federspiel and a bioengineering doctoral student.