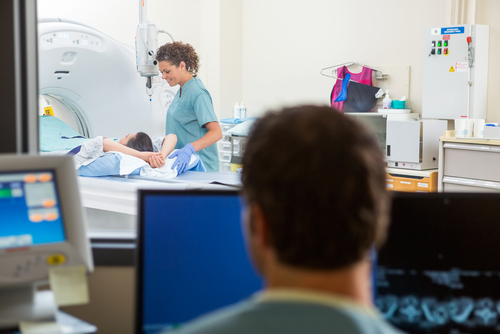
 Medicare yesterday announced a final decision that it will start paying for computed tomography (CT) lung cancer screening in high risk patients, including people between the ages of 55 and 74 who have smoked at least a pack a day for 30 years, or the equivalent. The decision is in line with recommendations made by physicians, associations, and stakeholders over the last few months.
Medicare yesterday announced a final decision that it will start paying for computed tomography (CT) lung cancer screening in high risk patients, including people between the ages of 55 and 74 who have smoked at least a pack a day for 30 years, or the equivalent. The decision is in line with recommendations made by physicians, associations, and stakeholders over the last few months.
The Center for Medicare & Medicaid Services (CMS) delivered a formal proposal this Monday, suggesting the full payment of CT scans, in order to improve early detection of the most deadly cancer in the world. A 30-day open comment period will follow the decision, which is expected to mark a major improvement in healthcare, as the current law does not require Medicare to cover the diagnostic tests.
“I think after a long effort to get to this point, CMS got it right,” said the president and CEO of Lung Cancer Alliance, Laurie Fenton Ambrose, to NBC News‘ Maggie Fox in a report yesterday. “This has the potential of being one of the most significant cancer mortality-reducing efforts to date. We are finally focusing on what is a quarter of all cancer, and that’s lung cancer.”
CT lung cancer screening is currently the first and only diagnostic method to have been proven effective in preventing the disease. Advocates believe it could save thousands of peoples’ lives annually with early detection, and health experts have already proven that the test, which costs between $100 and $400, may be able to prevent 20% of lung cancer-related deaths, making it as comparable to other preventive exams, such as mammograms or colonoscopies.
“We are going to see the meter move on cancer’s mortality. It’s an extraordinary time for our community and we are thrilled. We are confident that, while a draft, it should remain intact,” Ambrose added. Even though many private insurers already covered the lung cancer screening, Medicare had been reluctant to commit to offering it for months, despite the recommendations and studies that demonstrated its efficacy and cost effectiveness.
[adrotate group=”3″]
The United States Preventive Services Task Force (USPSTF) recommended that heavy smokers should receive regular lung cancer screening, revealing that the test was cost effective, and advising Medicare to cover the exam. The task force review, conducted in collaboration with Milliman, Inc., and based on National Lung Screening Trial data, also revealed that the test is more effective than other screening programs, and has statistically shown that it saves more lives than automobile seat belts or airbags.
The high mortality rate associated with lung cancer is related to the fact that the symptoms only appear when the disease has already spread. Lung cancer kills about 160,000 people every year, according to the numbers of the American Cancer Society. Therefore, several healthcare, patient, and advocacy associations lobbied for and are now celebrating Medicare’s coverage of the exam.
“Medicare coverage provides access to care for seniors and will help physicians save thousands of lives each year from the nation’s leading cancer killer,” said Dr. Ella Kazerooni, chair of the American College of Radiology Lung Cancer Screening Committee. “We strongly advise older current and former heavy smokers to speak with their doctors about whether CT lung cancer screening is right for them. If they and their doctor decide that screening is warranted, we encourage patients to seek out an ACR lung cancer screening center.”
The National Cancer Institute had already confirmed the effectiveness of CT scans in a recent study, which was reanalyzed after Medicare questioned the coverage of CT scans in older and high risk patients. The study revealed that the exam is beneficial in early detection, even for heavy smokers older than 65 years older, which corroborated the results of a first study that demonstrated the higher probability of older patients to register false-positives, as well as to develop the disease.