 A research group in Ontario, Canada has found that over-reliance on pulse oximetry readings may contribute to unneeded hospital care. The study appeared in the August 20th issue of the Journal of the American Medical Association (JAMA).
A research group in Ontario, Canada has found that over-reliance on pulse oximetry readings may contribute to unneeded hospital care. The study appeared in the August 20th issue of the Journal of the American Medical Association (JAMA).
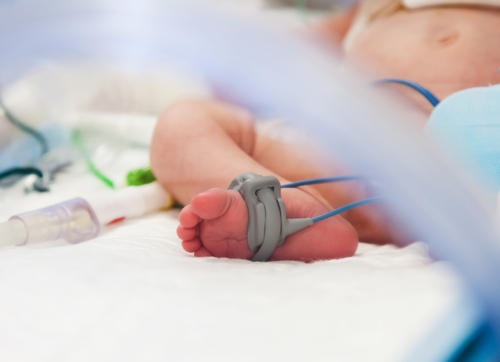
Pulse oximetry is a method for monitoring oxygen saturation. Oxygen saturation refers to the amount of oxygen that the red blood cells are carrying through the circulatory system, and is measured as a percentage of the blood cells carrying oxygen. During pulse oximetry, a clinician places a sensor device on a region of the patient’s body, usually an earlobe or fingertip in an adult, or the foot in an infant. The device emits light through the body part, the light passes through pulsing blood and a detector can then measure an approximation of the oxygen being used.
The scientists, lead by Suzanne Schuh, MD, from The Hospital for Sick Children and Alberta Children’s Hospital in Canada, wanted to see the extent to which oximetry is being relied on as an indicator of when to hospitalize pediatric patients. They studied infants with bronchiolitis and artificially elevated oximetry measurements (by 3%) compared to infants who had true measurements of oxygen saturation.
The study took place from 2008 to 2013 in a pediatric emergency department and the scientists studied 213 otherwise healthy infants who were between the ages of 4 weeks to 12 months. The infants had bronchiolitis and actual oxygen saturations measured at 88 percent or higher.
[adrotate group=”3″]
They found that hospitalizations were indeed significantly affected by the oximetry measurements. Forty-four of 108 patients (41%) in the true oximetry group and 26 of 105 (25%) in the artificially elevated oximetry measurement group were hospitalized within 72 hours of the test. Patients with the true oxygen saturation values utilized more resources within 72 hours. No adverse patient outcomes were recorded in either group.
The authors of the study concluded that “Among infants presenting to an emergency department with mild to moderate bronchiolitis, those with an artificially elevated pulse oximetry reading were less likely to be hospitalized within 72 hours or to receive active hospital care for more than 6 hours than those with unaltered oximetry readings. This suggests that oxygen saturation should not be the only factor in the decision to admit, and its use may need to be reevaluated.”
The study indicates that physicians may over-rely on oxygen saturation as a measurement for determining whether or not to admit pediatric patients to the hospital. The 3% oxygen saturation increase led to the perception that oxygen use was better than it actually was and was a major motivator for the decision to not to hospitalize. In the true oximetry patients, hospitalization increased, but no adverse outcomes were recorded. Clinicians should ideally use additional measurements with oximetry to more accurately assess the risk for adverse outcomes associated with bronchiolitis.