Most people in the developing world who live with asthma, cystic fibrosis, or other chronic lung diseases have no way of measuring the status of their lung function outside of clinic or doctor visits.
Most people in the developing world who live with asthma, cystic fibrosis, or other chronic lung diseases have no way of measuring the status of their lung function outside of clinic or doctor visits.
However, it occurred to a team of scientists at the University of Washington (UW) in Seattle that many of these people do have access to a telephone, though perhaps not a late model app-driven smartphone — more likely a decade-old flip-phone or a communal village landline.
That reality inspired the UW computer science, engineering, and electrical engineering researchers to develop a sensing device called SpiroCall, which can accurately measure lung function over a simple phone call from any type of phone.
A paper titled “SpiroCall: Measuring Lung Function over a Phone Call,“ was recently presented at the Association for Computing Machinery’s CHI 2016 conference in San Jose, California, and showed that SpiroCall’s results come within 6.2 percent of matching results from clinical spirometers used in hospitals and doctors’ offices, meeting the medical community’s accuracy standards. Due to variability in the ways particular patients exhale during spirometry tests, the industry considers anywhere in a range from 5 to 10 percent to be within an acceptable margin of error.
Researchers noted that cost and accessibility have been logistic obstacles impeding the adoption of spirometers (devices that measure lung function) in the developing world outside of clinical settings, especially in low-resource environments. A smartphone app previously developed by the UW led team 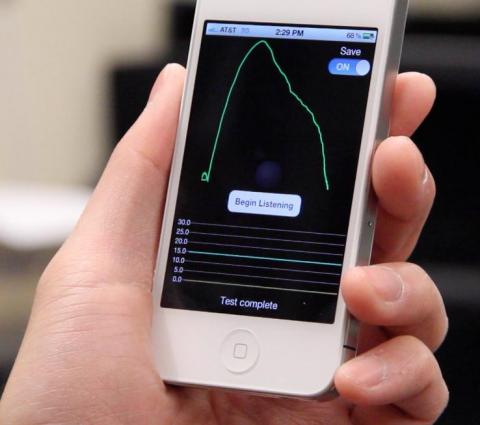 called SpiroSmart used the smartphone device’s built-in microphone as a spirometer, but people in low- or middle-income countries do not often have access to smartphones.
called SpiroSmart used the smartphone device’s built-in microphone as a spirometer, but people in low- or middle-income countries do not often have access to smartphones.
In their paper, the team reported how spirometry can be performed from any telephone using the standard telephony voice channel to transmit the sound of the spirometry effort. Researchers investigated how using a 3D-printed vortex whistle can affect accuracy of common spirometry measures and mitigate usability challenges.
This research led to the development of a new device called SpiroCall. Its performance was evaluated in a study with 50 participants against two gold standard medical spirometers. Based on the results, the researchers concluded that SpiroCall has an acceptable mean error when used with or without a whistle for performing spirometry, and advantages of each are discussed in the paper.
 “We wanted to be able to measure lung function on any type of phone you might encounter around the world — smartphones, dumb phones, landlines, pay phones,” said Shwetak Patel, a Washington Research Foundation Endowed Professor of Computer Science & Engineering and Electrical Engineering at UW, in a press release. “With SpiroCall, you can call a 1-800 number, blow into the phone, and use the telephone network to test your lung function.”
“We wanted to be able to measure lung function on any type of phone you might encounter around the world — smartphones, dumb phones, landlines, pay phones,” said Shwetak Patel, a Washington Research Foundation Endowed Professor of Computer Science & Engineering and Electrical Engineering at UW, in a press release. “With SpiroCall, you can call a 1-800 number, blow into the phone, and use the telephone network to test your lung function.”
Patel directs his UW research group, the Ubicomp Lab, whose focus is the development of new sensing systems, energy and water sensing, mobile health, and new interaction technologies. Named top innovator of the year by Seattle Business Magazine and Newsmaker of the Year by Seattle Business Journal in 2011, Patel’s past work was also honored by The New York Times as a top technology of the year in 2005. He is a member of the World Economic Forum’s Global Shapers Community, and was selected as a Seattle Shaper in March 2012 — the same year UbiComp Lab introduced the smartphone app SpiroSmart.
Patients using SpiroCall take a deep breath in, and then exhale as vigorously and quickly as they can until they are unable to exhale any more. The phone’s microphone senses sound and pressure from the exhalation, and sends the data to a central server, which uses machine learning algorithms to convert the data received into standard lung function measurements.

“People have to manage chronic lung diseases for their entire lives,” said the study’s lead author, Mayank Goel, a UW computer science and engineering doctoral student. “So there’s a real need to have a device that allows patients to accurately monitor their condition at home without having to constantly visit a medical clinic, which in some places requires hours or days of travel.”
Over the past four years, the Ubicomp Lab-based team has collected data from more than 4,000 patients attending clinics in Seattle and Tacoma, Washington, as well as in India and Bangladesh, where clinicians have measured lung function using both SpiroSmart and commercial spirometers. The resulting data was harnessed to improve machine-learning algorithms performance, and lay the groundwork for the team’s current FDA clearance process.
However, in surveying patients from India and Bangladesh, it dawned on the team that a significant percentage of people in those countries did not own smartphones and would be unable to use SpiroSmart in their own homes, which negated a key goal of their project. Noting that the only smartphone sensor they were actually using was the device’s microphone, a component all phones have in common, the researchers decided to develop a system that would work with any type of telephone, anywhere in the world, through a patient call-in service.
The resulting SpiroCall device transmits collected audio using a standard phone channel as opposed to a sound file transferred by a smartphone app over the internet. The team was able to combine multiple regression algorithms in order to provide reliable lung function estimates despite the degraded audio quality of phone lines.
 “We had to account for the fact that the sound quality you get over a phone line is worse,” explained paper co-author and UW electrical engineering doctoral student Elliot Saba. “You can imagine how listening to someone play a song over a phone line would sound compared to listening to it on your music app; there’s a similar difference with a spirometry test.”
“We had to account for the fact that the sound quality you get over a phone line is worse,” explained paper co-author and UW electrical engineering doctoral student Elliot Saba. “You can imagine how listening to someone play a song over a phone line would sound compared to listening to it on your music app; there’s a similar difference with a spirometry test.”

The research team also developed the 3D printed whistle designed to address training challenges by enabling patients to hear what a good test sounds like. The whistle, which changes pitch when the patient exhales and can be used in conjunction with SpiroCall, also improved test performance for very ill patients whose vocal cords are unable to generate enough sound for the phone’s microphone to pick up.
Future objectives for the Ubicomp Lab research team include additional data collection, and determining how to best communicate test results in a way that will make sense to patients.
“Our research area is not just about sensing, but human-centered sensing,” Goel said. “Because this project has been around for four years, we’ve been able to talk to a lot of patients about how they’re able to use the technology, and that feedback has really helped us make smart improvements.”
The research was funded by the Life Sciences Discovery Fund, the Wallace H. Coulter Foundation, and the University of Washington.
Members of the research team and paper authors include UW electrical engineering doctoral student Josh Fromm; UW computer science and engineering doctoral student Eric Whitmire; former high school intern and California Institute of Technology freshman Maia Stiber; Southern Methodist University assistant professor of computer science and engineering Eric Larson; and the late Gaetano Borriello, UW professor of computer science and engineering.