I still remember the day I found out I needed to use supplemental oxygen.
It was June 2014. I had gone to a follow-up appointment with my pulmonologist after he prescribed a six-week course of prednisone to reduce inflammation in my lungs. My lungs were harmed by the chemotherapy and radiation I received for treatment of breast cancer. I was upbeat, and felt like the prednisone had helped a little, but had no idea of the seriousness of my disease.
I met with the doctor, gave him an update, and made an appointment for another three months. Before I left, he sent me down the hall to do the “six-minute walk” test. This is the test where they have you walk for six minutes while wearing an oximeter on your finger in order to measure how much oxygen is in your blood as you exert yourself.
I failed this test, registering 84% O2 saturation after only three minutes of walking. My first clue there was a problem was when the alarm went off on the oximeter, and two nurses came rushing over to me to catch me in case I fainted. I felt fine, and was wondering what all the hullabaloo was about. The nurse said the doctor wanted to talk with me before I left. I said, “No, I’ve already seen him, and he said I could leave after this test.” She said “No, he needs to see you.”
I sat in his office wondering what was going on.
When he came back in, he said, “You need to use oxygen.” I said, “What? What are you talking about?” He then explained that I needed to use supplemental oxygen whenever I walked anywhere. He didn’t explain what was going on with my lungs, he just handed me a prescription for it and told me the oxygen company would be calling me and bring me what I needed the next day.
I said, “You want me to push a canister around when I’m walking as if I’m an 80-year-old woman (I was 58)?” He said, “Yes.” I said, “I’m not going to do that. You need to come up with a different option.” He looked shocked at my response, and then offered me the option of prescribing a portable oxygen concentrator that I could wear in a bag over my shoulder. I said that I was willing to give that a try.
He then asked me to go to the next building to get a CT scan of my chest. He wanted me to push his little tank of oxygen over there, but I told him, “No thanks, I’m fine walking over there on my own.” As I look back, I am shocked that he didn’t explain what was happening to my lungs that necessitated supplemental oxygen, or offer any acknowledgement of my distress.
Here’s what I wish he’d said to me:
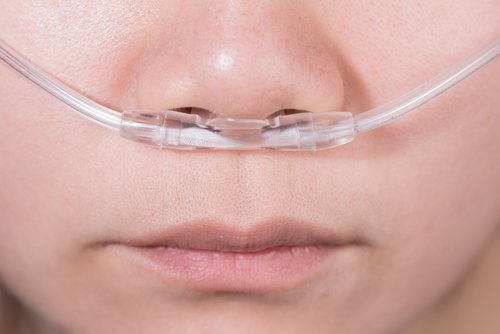
“I’m so sorry to tell you that your lungs have gotten worse since we met. It looks like the prednisone helped a little, but your lungs are still really struggling. They are inflamed and have some scarring in places that air used to go into. Because of this, your lungs cannot take in enough air to send to the rest of your body. In order for your body and brain to stay healthy, you’ll need help getting more oxygen than your lungs can provide. The way we do this is to give you supplemental oxygen to breathe. This way your body gets air both from your lungs, and from this tube we call a ‘nasal cannula.’ You won’t need to use this when you are sitting, just when you are moving around.
“I know this is quite a shock and you are trying to make sense of what I’m telling you. I’m so sorry to deliver this awful news. Do you have any questions about what I’ve said so far?
“There are two main ways for you to use supplemental oxygen when moving around. You can push one of these tanks around and go wherever you want. You can also carry a portable oxygen concentrator in a bag, on your shoulder, or in a backpack. This is a small machine that takes in room air and gets rid of the nitrogen and other gases in the air, concentrates the oxygen to a higher level and sends it back to you to breathe. I can order either one to be delivered to your home tomorrow. Which one would you like?”
What a difference it would have made to get a kind and informative explanation like this!
How about you? How were you told that you needed to use supplemental oxygen? What was that experience like? What did you like about how you were told, and what do you wish had been different?
Next week I’ll be sharing more about supplemental oxygen, and what I’ve learned about the different options out there. Please leave me questions you’d like answered in the comments section below.
Please share this post with anyone you feel could benefit, or on social media. We’re in this together.
***
Note: Pulmonary Fibrosis News is strictly a news and information website about the disease. It does not provide medical advice, diagnosis, or treatment. This content is not intended to be a substitute for professional medical advice, diagnosis, or treatment. Always seek the advice of your physician or other qualified health provider with any questions you may have regarding a medical condition. Never disregard professional medical advice or delay in seeking it because of something you have read on this website. The opinions expressed in this column are not those of Pulmonary Fibrosis News, or its parent company, BioNews Services, and are intended to spark discussion about issues pertaining to pulmonary fibrosis.

I had stage 4 melanoma I’ve been free for almost 2 year’s but then I got leginella followed by a lung fungi. I didn’t get put on oxygen off cops or cancer it wasn’t till after the leginella still on it after 8 months
I have been having this issue for almost two years. Guess I need to go to a pulmonary doctor.
My husband was diagnosed with PF a year ago January…he was told oxygen would not do him
any good. As time goes on, he is breathing
slower all the time, feeling lethargic and
not able to do hardly anything….sleeping a lot. He is 77 years old and has been a hard
working farmer all his life. This is so devastating to us and we feel there are no answers to helping him at this time. Any help would be greatly appreciated.
My first visit to the pulmonologist, he told me I would likely need a lung transplant. I thought I had pneumonia!
My lung test showed I have 43% good in my lung function…do u think that is s good percentage??? Ty
I’ve been on oxygen 24\7 since April 2015. I’m on 3 expensive inhalers, that’s my meds,if I start to swell up I take water pills. I can’t do my housework like I use to, I did sign up, and my insurance is paying for, a exercise class that has helped me a lot, but I’m about 3 weeks this class will end, and my health will go down as a result of it. The class helped my breathing, to were I can do more . Please any advice could be helpful.
I have to use oxygen mostly at night. But have found i need it sometimrs during the day, i have COPD i know i shouldn’t but i still smoke maybe about 2-3 cigs a day. Is this dangerous disgustful smoke, poison going thtough my tank and delivering to me throigh my cannula?
How do you pay for the portable small one you carry? Ins, Medicare? I was going to buy one but I found out they don’t last long and very expensive, this was several yrs ago.
I knew that I would be needing supplemental oxygen (I attend a support group and knew that people used their oxygen), and when given the hall test, that became obvious to everyone. However, I was told it was “as needed” and when I walked. When they brought the POC out, I said “Don’t you have one of those smaller ones?”. I needed 6L for walking and they had brought a canister that I pull behind me. It gives 6L of pulses. I was very disappointed as I didn’t know that I couldn’t have something smaller. As it is, when I walk, those 6L of pulse, barely keep my oxygen levels up to where they should be.
It is ridiculous that the physician didn’t explain oxygen saturation and the measurement by the pulse oximeter. Would have made a lot more sense to her then.