 A recent study from the University of Manchester (UM) revealed how a blood sample from lung cancer patients can help monitor and predict the body’s response to treatment. This finding gives researchers new clues for developing next-generation personalized medications for each patient.
A recent study from the University of Manchester (UM) revealed how a blood sample from lung cancer patients can help monitor and predict the body’s response to treatment. This finding gives researchers new clues for developing next-generation personalized medications for each patient.
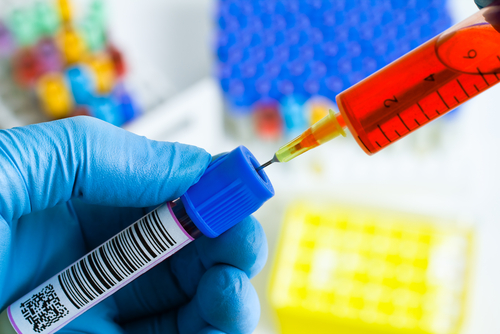
Researchers focused on the potential of pinpointing circulating tumor cells (CTC), which are cells that loosen up from the tumor and circulate through the blood, as a way to explore the disease with minimally invasive methods. The trial was conducted at the Cancer Research UK’s Manchester Institute, based at the UM.
Patients with small cell lung cancer (SCLC) had a much higher amount of CTC in a sample of blood than patients with other types of tumors. Additionally, the researchers, in collaboration with lung specialists and oncologists, have identified a correlation between the number of CTC in the blood and the survival rate, since patients with fewer cells lived longer.
SCLC is not only aggressive, but it registers poor survival rates. One of the obstacles to proper treatment is the inoperability of the tumor and difficulty in attaining biopsies, which results in a lack of samples for scientists to work on.
“Access to sufficient tumour tissue is a major barrier to us fully understanding the biology of SCLC. This liquid biopsy is straightforward and not invasive so can be easily repeated and will allow us to study the genetics of each lung cancer patient’s individual tumour. It also means that we may have a feasible way of monitoring patient response to therapy, hopefully allowing us to personalize and tailor individual treatment plans to each patient,” said Prof. Caroline Dive, who led the study.
Researchers were also able to create CTC tumor models in mice that are called CTC-derived explants (CDXs). The experiment with mice and chemotherapy showed the same results as the ones from donor patients.
In the study, published in the journal Nature Medicine, a new method was developed for testing innovative therapies in the lab and conducting further investigations in order to increase knowledge about tumors’ resistance to drugs.
“We can use these models to help us understand why so many SCLC patients acquire resistance to chemotherapy and to search for and test potential new targeted treatments,” added Professor Dive.