 For a disease that not so long ago was a major cause of series illness and death in our society, pneumonia is discussed relatively little these days, at least in the developed world, and even in the medical community.
For a disease that not so long ago was a major cause of series illness and death in our society, pneumonia is discussed relatively little these days, at least in the developed world, and even in the medical community.
The non-profit watchdog Decoded Science reports that pneumonia is among the top five conditions searched on Wikipedia by doctors last year.
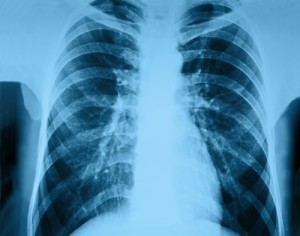
Pneumonia is a lung inflammation affecting primarily microscopic air sacs known as alveoli, and is usually caused by infection with viruses or bacteria and less commonly other microorganisms, certain drugs and other conditions such as autoimmune diseases. Typical pneumonia symptoms include coughing, chest pain, fever, and difficulty breathing. Treatment depends on the underlying cause. Pneumonia presumed to be bacterial is treated with antibiotics. If the pneumonia is severe, the affected person is, in general, admitted to hospital.
Pneumonia still reportedly afflicts some 450 million people globally per year, seven percent of humanity, and results in about 4 million deaths, mostly in underdeveloped countries, and the global economic cost of community-acquired pneumonia has been estimated at $17 billion annually worldwide.
Wikipedia notes that pneumonia has been a common disease throughout human history, its symptoms having been described by Hippocrates (c. 460 BC – 370 BC), and even he referred to it as a disease “named by the ancients.” Maimonides’ (1135–1204 AD) description of the basic symptoms that occur in pneumonia is quite consistent to those found in modern textbooks, and reflected the extent of medical knowledge through the Middle Ages into the 19th century, when Edwin Klebs was reportedly the first to observe bacteria in the airways of persons having died of pneumonia in 1875. Sir William Osler, known as “the father of modern medicine,” described pneumonia as the “captain of the men of death” in 1918,
However, with the mid-20th Century discovery of penicillin and other antibiotics, modern surgical techniques, and intensive care in the second half of the 20th Century, mortality from pneumonia, which had typically approached 30 percent, dropped precipitously in the developed world, and pneumonia’ prominence as a major public health concern decreased.
Due to the still high burden of pneumonia pathology in developing countries, and a relatively low awareness of the disease in developed countries, the global health community has declared 12th November as World Pneumonia Day to advocate that concerned citizens and policymakers to take action against the disease as a still potent agent of human misery.
 A team of researchers at the University of Michigan Medical School in Ann Arbor, Michigan, observe that while pneumonia remains a major cause of morbidity and mortality, no new methods of treatment have entered clinical practice since the discovery of antibiotics, development of which has stagnated while drug-resistant pathogenic organisms are becoming increasingly common, and and no novel treatment methods for management of pneumonia have been incorporated into practice since the beginning of antibiotic therapy 75 years ago.
A team of researchers at the University of Michigan Medical School in Ann Arbor, Michigan, observe that while pneumonia remains a major cause of morbidity and mortality, no new methods of treatment have entered clinical practice since the discovery of antibiotics, development of which has stagnated while drug-resistant pathogenic organisms are becoming increasingly common, and and no novel treatment methods for management of pneumonia have been incorporated into practice since the beginning of antibiotic therapy 75 years ago.
Nevertheless, scientific knowledge about lung ecology has advanced in the past 70 years, and the UoM scientists observe in a paper published in the journal Lancet Respiratory Medicine that innovations in culture-independent microbial identification techniques have shown that the lungs, previously deemed sterile in the absence of infection, actually contain diverse and dynamic communities of microbes.
In their Lancet article, entitled “Towards an ecology of the lung: new conceptual models of pulmonary microbiology and pneumonia pathogenesis” (The Lancet Respiratory Medicine, Volume 2, Issue 3, Pages 238 – 246, March 2014 doi:10.1016/S2213-2600(14)70028-1) Drs. Robert P Dickson MD and John R Erb-Downward PhD of the Division of Pulmonary and Critical Care Medicine, Department of Internal Medicine, University of Michigan Medical School, and colleague Dr. Gary B Huffnagle PhD also associated with the school’s Department of Microbiology and Immunology argue that their observations have highlighted the inadequacy of traditional conceptual models of lung microbiology and the pathogenesis of pneumonia, hampering progress in research and practice.
Borrowing pivotal concepts from the fields of ecology and complexity theory, the University of Michigan scientists propose three new conceptual models to replace the traditional models of lung microbiology: 1) an adapted island model of lung biogeography; 2) the effect of environmental gradients on lung microbiota; and 3) pneumonia as an emergent phenomenon propelled by unexplored positive feedback loops.
Drs. Dickson, Erb-Downward, and Huffnagle consider the respiratory tract a single ecosystem extending from the nares to the alveoli, comprising a continuous, and continuously varying, microbial topography, observing that the number of microbial species at a given site in the respiratory tree is an integrated function of many immigration and extinction factors, and that an ecosystem of lung microbiota has all of the features of a complex adaptive system: diverse entities interacting with each other within a common space, showing interdependent actions and possessing the capacity to adapt to changes in conditions. They note that complex adaptive systems are fundamentally different in behavior from the simple, linear systems typified by the traditional model of pneumonia pathogenesis, and call for distinct analytical approaches.
Drs. Dickson, Erb-Downward, and Huffnagle contend that traditional conceptual models of lung microbiology are inadequate, as shown by observations using culture-independent techniques of bacterial identification, and that by using pivotal concepts from the fields of ecology and complexity theory, their three innovative conceptual models for the study of lung microbiology provide a theoretical framework for development of novel approaches to understanding of the pathogenesis, prevention, and treatment of respiratory infections.
Sources:
The Lancet Respiratory Medicine
Wikipedia
Decoded Science

