 Bronchiectasis and chronic obstructive pulmonary disorder (COPD): synonyms for the same condition? Not quite. The American Thoracic Society defines COPD as “a group of lung conditions that make it difficult to empty the air out of the lungs.” While bronchiectasis, which is characterized by permanent enlargement of bronchi and bronchioles, may lead to obstructed breathing from abnormal mucus production like COPD, evaluation and treatment for both diseases differ.
Bronchiectasis and chronic obstructive pulmonary disorder (COPD): synonyms for the same condition? Not quite. The American Thoracic Society defines COPD as “a group of lung conditions that make it difficult to empty the air out of the lungs.” While bronchiectasis, which is characterized by permanent enlargement of bronchi and bronchioles, may lead to obstructed breathing from abnormal mucus production like COPD, evaluation and treatment for both diseases differ.
“Chronic obstructive pulmonary disease and bronchiectasis are different but related diseases that occur separately, but can coexist,” wrote Drs. Shannon A. Novosad and Alan F. Barker, both of Oregon Health and Science University, in “Chronic Obstructive Pulmonary Disease and Bronchiectasis,” published in Current Opinion in Pulmonary Medicine. Yet, the chances of concurrent COPD and bronchiectasis are slim: while COPD is the third leading cause of American death, bronchiectasis can be considered an orphan disease that affects approximately 110,000 Americans.
However, in one study published in Egyptian Journal of Chest Disease and Tuberculosis, “Bronchiectasis in COPD Patients,”47.8% (33 of 69) of enrolled participants had both bronchiectasis and COPD. The researchers behind the study identified that severe functional impairment, defined as a forced expiratory volume in one second (FEV1) of less than 50%, correlated to developing bronchiectasis, just as greater bacterial colonization and exacerbation rate did, as well.
[adrotate group=”6″]
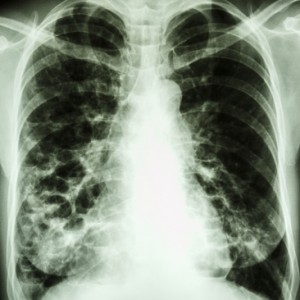
It can be easy to mistake one disease for the other. Both diseases have symptoms of dyspnea (shortness of breath), chronic cough, potential for daily sputum production, and airflow obstruction. Methods for determining the reason for these symptoms begin with patient history and clinical examination. Patients with COPD commonly have chronic sputum production associated with coughing, yet bronchiectasis patients may have either a dry or wet cough.
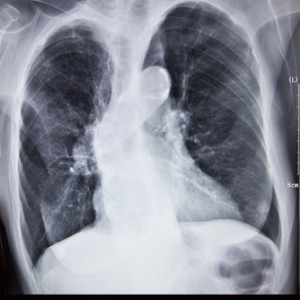
As more quantitative measures, lung function and imaging tests are also useful in diagnosing the diseases. COPD is confirmed by a post-bronchodilator FEV1 less than 80% with an FEV1/forced vital capacity (FVC) less than 70%. Bronchiectasis can initially mimic these COPD features, but as bronchiectasis progresses, progressive lung damage can lead to mixed lung function results. Accordingly, thoracic computed tomography (CT) scans are considered the gold standard to diagnose bronchiectasis. A large internal bronchial diameter, thickened bronchial wall, and altered airway geometry evident through CT scans are all indicators of possible bronchiectasis. Imaging results for COPD validate functional tests by highlighting centrilobular emphysema, given that the cause is smoking-related.
It is vital to diagnose one disease versus the other in patients, as “in the early stage of disease [it] is extremely important for the adoption of appropriate therapeutic measures,” according to “Airway Disease: Similarities and Differences between Asthma, COPD and Bronchiectasis,” published in Clinics. Treatments for COPD and bronchiectasis are designed to address the unique causes and risk factors for disease. Whereas COPD is largely associated with lung irritants such as pollution and smoking, bronchiectasis is often a result of respiratory infections or lung transplantation. Some cases of disease can also be associated with host factors including alpha-1 antitrypsin deficiency and other host factors, leading new treatments in the pipeline to take a more genetics-based approach.
In both diseases, the body’s natural inflammatory response involves neutrophils, macrophages, and CD8 T-cells as the primary cell types responsible for trying to attenuate damage in the airways. Consequently, COPD is often treated with anti-inflammatory drugs, such as inhaled corticosteroids. However, bronchiectasis often requires an antibacterial approach to stop the vicious cycle of impaired ciliary function leading to bacterial colonization and thick mucus accumulation, leading to inflammation and impairment of mucociliary clearance.
Differing treatment goals also motivate the use of different therapeutic regimens. Whereas “COPD therapy is directed primarily to the relief of symptoms and the prevention of disease progression,” wrote Dr. Rodrigo Anthanazio, of Heart Institute (InCor) in Sao Paulo, Brazil, “In bronchiectasis, the primary goal of treatment is to prevent disease progression and improve the quality of life and symptoms.” At times, intervention for COPD can be as simple as smoking cessation, but first-line treatment usually consists of using short-acting beta2-agonists (SABAs) to dilate the airways. While it may seem counter intuitive to use SABAs to treat bronchiectasis, some studies have combined long-acting beta2-agonists (LABAs) with inhaled corticosteroids and shown benefits for patient quality of life scores.
Despite available treatments, a commonality of both COPD and bronchiectasis is a high hospitalization rate. The most recent data published in the Chest article “Hospital Discharges, Readmissions, and Emergency Department Visits for Chronic Obstructive Pulmonary Disease or Bronchiectasis among US Adults: Findings from the Nationwide Inpatient Sample 2001-2012 and Nationwide Emergency Department Sample 2006-2011” indicates that the rate of hospitalization has remained steady for more than 10 years. Over 240 of 100,000 individuals are hospitalized with either COPD or bronchiectasis, and emergency department visits number close to 1.5 million per year.
At times, it can be difficult to directly compare bronchiectasis and COPD, as research specific for bronchiectasis is sometimes scarce. A predicted increase in research comes as a double-edged sword because the increase is warranted due to an increased rate of disease occurrence in the population, despite efforts to mitigate airway disease. As more studies are conducted, the similarities and differences between bronchiectasis and COPD will continue to become more well defined.
[adrotate group=”6″]
Sources:
American Thoracic Society. What Is Chronic Obstructive Pulmonary Disease (COPD)? [Internet]. New York (NY): American Thoracic Society; c1998-2014 [cited Jan 21 2014]. Available from: http://www.thoracic.org/clinical/copd-guidelines/for-patients/what-is-chronic-obstructive-pulmonary-disease-copd.php
Novosad SA, Barker AF. Chronic obstructive pulmonary disease and bronchiectasis. Current Opinion in Pulmonary Medicine, 2013;19(2):133-139.
Arram EO, Elrakhawy MM. Bronchiectasis in COPD patients. Egyptian Journal of Chest Disease and Tuberculosis, 2012;61(4):307-312.
Athanazio R. Airway disease: similarities and differences between asthma, COPD and bronchiectasis. Clinics (San Paulo), 2012;67(11):1335-1343.
Ford ES. Hospital discharges, readmissions, and emergency department visits for chronic obstructive pulmonary disease or bronchiectasis among US adults: findings from the Nationwide Inpatient Sample 2001-2012 and Nationwide Emergency Department Sample 2006-2011. Chest, 2014:14-2146.

Thank you for your post. I have bronchaiectis and find myself on occasion going to the ER with shortness of breath. To me it feels like Asthma but they always say they don’t hear the wheezing . The difficulty is in my upper chest into my throat. What shall I call it? The abuterall treatment they give helps settle it down. I need a name for what is happening .. it’s not Asthma then there should be a term I can use so they understand.
I wonder if you are not experiencing mild/moderate tracheolmalacia? My daughter was recently diagnosed.
I was diagnosed with brochiecstasis a month ago after a long period of being told I had asthma. For me it has been referred to as episodes. I kept telling the doctors my chest rattles and they interpreted that to mean whizzing….it isn’t wheezing it is a rattle. The only treatment that has helped me are antibiotics and cortisone. So far nothing has helped me catch my breath during an episode. It is very scary.
hi my partner is currently in the early stages of finding out that she has bronchiectasis, i found your info very usful in understanding what Bronchiectasis is.
Thank you a reply would be great
What is the difference in prognosis between COPD and bronchietasis?
the difference between COPD and bronchiectasis?
I am 91 years old . For over 10 years I was told I had COPD
but I detected that the doctors I saw were not confident in the
diagnosis. Eventually I saw a Consultant who said the evidence after many tests was somewhat clear and also not so clear and ordered a CT Scan after which he told me I had mild bronchiectasis and late onset asthma and I continued using inhalants . I have had several admissions to hospital with severe chest infections and the last hospital consultant I saw after a CT scan said he saw no evidence of bronchiectasis. Treatment for infections was always with antibiotics and short course
steroids . Confusion reigns. I was relieved to see from this site that the link between COPD and bronchiectasis is still not totally explained.
I have Bronchiectasis and what appears to be asthma,,this year I have been on Steroids and Antibiotics 6 times. It is now Spring and I gave a terrible cough, loads of white frothy sputum and runny nose,,,could this be blossom allergies..thank you and do Brochiectasis and allergies go together
In 2016 my sister in-law told us about Rich Herbs Foundation (ww w. richherbsfoundation. c om) and their successfully COPD treatment. We ordered the COPD Formula product after reading positive reviews from other patients who used the treatment, i am happy to report this COPD treatment reversed my lungs condition and damage. My quality of life has greatly improved and every one of my symptoms including difficulty breathing, Chronic cough and wheezing are gone. I will be 52 soon and have never been healthier.
I have mild bronchiectasis. Also lung function test show I only blow 14 % if the value. So doctors say I have severe lung disease and it is COPD. u have breathlessness and can’t walk for 8 months. I never smoked but worked as a photographer near the fire training classes where artificial wood fires weremail made to train people. It was on a massive open ground. Could this be a reason that I inhaled smoke ?. Doctor say mild bronchiectasis can’t give so much breathing get problem. I mean confused.
I have bronchiectasis
2 yrs now I have no cough just too much sputam coming up after I eat and all day long
clearing my throat
most uncomfortable.I can t take antibiotics
too many side effects
any suggestions appreciated Thank you
I’ve been suffering bouts of coughing with White Sputum for 12 years. Firstly I was diagnosed with Asthma and prescribed inhalants – no improvement. I’m still coughing and still spitting what seems to be White glare. My social life is down to Zero. It’s worse when I lie down in the evening.