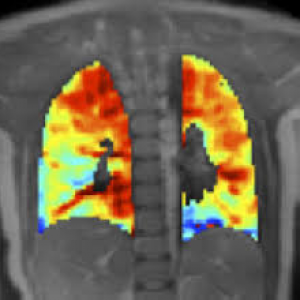
 A new study assessed the feasibility and reproducibility of dynamic oxygen-enhanced magnetic resonance imaging (OE-MRI) as a non-invasive, non-ionizing imaging technique with the capability to assess regional lung function in asthma. The study entitled “Dynamic oxygen-enhanced magnetic resonance imaging of the lung in asthma—Initial experience” was published in the European Journal of Radiology by Wei-Juan Zhang part of Dr. Josephine H. Naish’s group at Centre for Imaging Sciences and Biomedical Imaging Institute, The University of Manchester, Manchester, UK, and colleagues.
A new study assessed the feasibility and reproducibility of dynamic oxygen-enhanced magnetic resonance imaging (OE-MRI) as a non-invasive, non-ionizing imaging technique with the capability to assess regional lung function in asthma. The study entitled “Dynamic oxygen-enhanced magnetic resonance imaging of the lung in asthma—Initial experience” was published in the European Journal of Radiology by Wei-Juan Zhang part of Dr. Josephine H. Naish’s group at Centre for Imaging Sciences and Biomedical Imaging Institute, The University of Manchester, Manchester, UK, and colleagues.
In most asthma studies the analysis has been focused on a component of lung function, such as ventilation, perfusion, or ventilation–perfusion mismatch, i.e. a defect which occurs in the lungs where ventilation (the exchange of air between the lungs and the environment) and perfusion (the passage of blood through the lungs) are not equivalent. It is potentially important to assess individual factors that contribute to functional impairment of the lungs, for example how oxygen (O2) is delivered and absorbed locally in the lung.
Dynamic oxygen-enhanced (OE-) MRI has been used to analyze alterations in lung function in several pulmonary disorders, but there is very little information about its efficacy in asthma. OE-MRI can provide spatial and temporal information on regional delivery and uptake of oxygen (O) in the lung by using O as a traceable agent. The paramagnetic O molecules, i.e. molecules that are attracted by a magnetic field, dissolve in the tissue water and blood plasma inside the lung and increase the lung spin-lattice relaxation rate (R), parameter that quantifies the rate of transfer of energy from the nuclear spin system, like oxygen, to the neighboring molecules, in proportion to dissolved O concentration and thus the local O partial pressure (PO).
[adrotate group=”3″]
The research team found that dynamic oxygen-enhanced (OE-) MRI is feasible in asthma and is sensitive to the severity of disease by distinguishing between mild and severe asthmatic groups and showing associations with lung function tests, and contributing to the monitoring of disease progress and evaluating the effects of treatment.
In other developments in respiratory health and asthma, a recent study published in The Journal of Allergy and Clinical Immunology showed that certain pulmonary features, before and after bronchodilation, are different according to the gender of the child. The study is entitled “Sex-related differences in pulmonary physiologic outcome measures in a high-risk birth cohort.”