A new study from Yale University has found that cells located along the walls of small blood vessels in the lung, called pericytes, promote the progression of idiopathic pulmonary fibrosis (IPF). The role these cells play in fibrosis previously had not been understood.
The study, “Human pericytes adopt myofibroblast properties in the microenvironment of the IPF lung,” was published in the Journal of Clinical Investigation Insight.
IPF is a type of lung disease whose cause is unknown. It is characterized by the presence of scarred and hardened tissue, called fibrotic tissue, in the lungs. Changes in the extracellular matrix, a network of diverse types of molecules that help bind cells together and regulate their function, have been associated with the disease.
Pericytes are cells located at intervals along the walls of capillaries, the smallest blood vessels in the body. These important cells are found in the body’s organs including the lungs, heart, and brain, and have been implicated in the development of tissue fibrosis.
The Yale research team set out to better understand the role these cells play in IPF, an approach that differs from that of other tissue engineers, who study cells in arteries and other larger blood vessels.
“We’re looking at these vessels because when IPF gets pretty bad, those small vessels go away and the tissue dies because there is limited nutrient and oxygen delivery to it,” Anjelica Gonzalez, associate professor of biomedical engineering and the study’s senior author, said in a press release.
To discover exactly what happens to this tissue, the investigators collected lung samples from IPF patients and analyzed the fibrotic lesions. They found that pericytes made up 15 to 21 percent of the lesions. No previous study had reported the presence of pericytes in these lesions, Gonzalez noted.
“Now we see that these blood vessel cells are still alive – they just become dysfunctional, as opposed to being supportive of healthy tissue,” Gonzalez said.
To better understand the mechanisms linking pericytes to the development of fibrosis, researchers engineered a human lung that could mimic the transition from healthy tissue to fibrotic tissue.
Using this lung model, investigators found that the cells were healthy as long as the tissue was soft and pliable. But when they were exposed to circulating factors, including the pro-inflammatory molecule TGF-beta1, the cells deposited proteins that caused tissue stiffness and scarring.
A key factor in the conversion from healthy to fibrotic behavior was a process called mechanosensing, which refers to the cells’ ability to sense physical forces transmitted by the surrounding extracellular matrix or neighboring cells.
Importantly, researchers found that this process could be disrupted with the administration of Boehringer Ingelheim’s IPF medication Ofev (nintedanib). Ofev’s effect on pericytes had not been demonstrated in previous studies.
“Our studies also present a potentially novel mode of action for the antifibrotic agent nintedanib,” the researchers wrote.
The next step will be to try to inhibit or reverse the fibrotic processes. The research team will test several therapies that already have been approved or are in the process of seeking approval, for their potential to revert diseased cells and tissues to a healthier state.
Ultimately, the findings may also contribute to the development of therapies that enable the formation of new vessels, the team said. Furthermore, this approach could also be applied to fibrosis of the skin, heart, and other tissues, Gonzalez added.

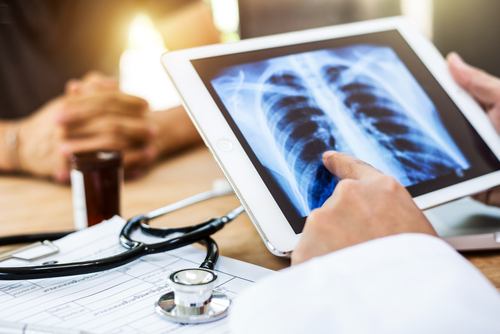
Information learned from this website has implied that the cells that keep the lungs healthy disappear when they are no longer fed healthy tissue. The Yale experiments and results to date are most encouraging. Let us hope that these continue and what a wonderful conclusion could occur if they come up with a solution to this loss of pericytes.
I feel that the ph 3 clinical trial that Prometic is doing with PBI-4050 & Ofev with 375 participants
What trial? Regenerative?
Prometic’s PBI-4050: Phase 3 Pivotal Clinical Trial Design For Idiopathic Pulmonary Fibrosis (IPF) Finalized
T.PLI | January 29, 2018
PR Newswire
LAVAL, QC, Jan. 29, 2018
Clinical trial design confirmed during FDA Type C meeting held on January 3, 2018
Simplified patient entry criteria to include IPF patients whether on background standard of care (i.e. nintedanib) or not
Primary endpoint analysis to be stratified on background therapy (+/- nintedanib)
Planned Interim analysis at 26 weeks
Company to host IPF KOL luncheon presentation and live webcast for the investment community on January 31 at 12 noon EST
LAVAL, QC, Jan. 29, 2018 /PRNewswire/ – Prometic Life Sciences Inc. (TSX: PLI) (OTCQX: PFSCF) (“Prometic”) announces today the outcome of a successful clinical development Type C meeting with the US Food and Drug Administration (FDA) for its orally active anti-fibrotic lead drug candidate, PBI-4050. The purpose of the meeting was to reach final agreement on the design of the Phase 3 pivotal clinical trial for PBI-4050 in patients with idiopathic pulmonary fibrosis (IPF).
Based on recommendations from the FDA, Prometic now will undertake an “all comers study”. The enrollment criteria will be greatly simplified such that the study will enroll patients with mild-to-moderate IPF, regardless of whether they are on background standard of care with nintedanib (OFEV®) or not. Therefore, the study will provide efficacy data on both PBI-4050 as a stand-alone agent, and as an add-on to nintedanib, and will be part of the dataset to support a simple, all-inclusive indication “for the treatment of IPF”. Patients will be randomized to receive placebo, or one of two doses of PBI-4050 (800 mg or 1,200 mg) for a total of 52 weeks. An interim analysis will be conducted at 26 weeks. The primary endpoint is the annual rate of decline in forced vital capacity (FVC), the total amount of air exhaled during a forced breath, expressed in mL and measured over 52 weeks (mL/year). Patients taking pirfenidone will be excluded because of a known drug-drug interaction between pirfenidone and PBI-4050.
“We are very pleased by the outcome of the meeting with the FDA. The recommendations provided by the FDA will allow us to conduct a clinical trial that is much more reflective of current treatment of IPF patients,” commented Dr. Joseph Parker, Senior Director, Prometic Clinical Affairs, who is overseeing the study. “This is going to be a multinational study, involving an experienced CRO in the field to help manage multiple sites across the United States, Canada, Australia, the UK and Europe. Our goal is to start patient enrollment mid-year.”
Pierre Laurin, President and Chief Executive Officer commented, “Prometic is now exceptionally well positioned to address the significant unmet medical needs in IPF. We have two late stage clinical candidates tackling different aspects of this devastating disease which affects more than 130,000 patients in the US alone. In addition to PBI-4050, we are pleased that Ryplazim™ was recently granted Orphan Drug Designation for IPF by the FDA. We are developing RyplazimTM to help manage the acute exacerbation episodes during which IPF patients accumulate hyaline membrane in the lungs, contributing to further significant loss of lung function.”